What is Thoracic Outlet Syndrome?
Thoracic Outlet Syndrome is a collective term for a group of individual syndromes which involves the compression of blood vessels and nerves around the thoracic outlet region.
General symptoms and signs include pain, paraesthesia (‘pins and needles’), and weakness and discomfort in the arm and shoulder. Also, symptoms can be aggravated by movement of the head and neck. Risk factors may include congenital anomalies, trauma and soft tissue change.
Where is the Thoracic Outlet?
The ‘Thoracic outlet’ is the narrow space between your collarbone and first rib, and it is where the brachial plexus (C5-T1) from the cervical spinal nerve and major blood vessels pass through. Anatomically, 3 spaces are classified as thoracic outlet. 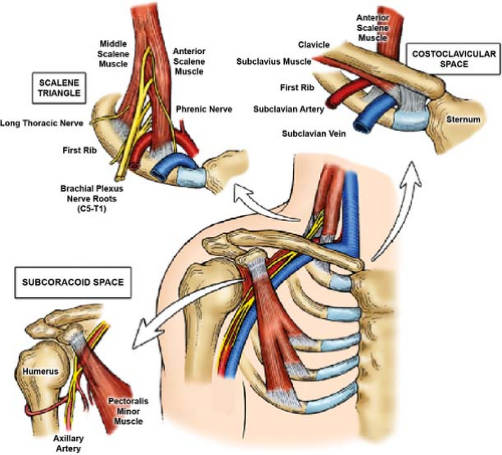
- Scalene Triangle
The border is formed by anterior scalene muscle (front), middle scalene (back) and 1st rib (floor)
- Costoclavicular Space
Similarly, the area is formed by the first rib and middle third of the clavicle.
- Subaracoid Space
It is the area beneath pectoralis minor tendon (near the coracoid process of the clavicle). The border is formed by: coracoid process (roof), pectoralis minor muscle (front) and 2nd-4th ribs (back)
Theses 3 spaces are potential sites of compression
- Scalene Triangle
- Lower roots of the brachial plexus and subclavian artery may be compressed due to hypertrophy or shortened anterior scalene muscle
- Costoclavicular space
- Subclavian vessels (artery and vein) and lower roots of brachial plexus can be compressed behind the clavicle in this space
- The costoclavicular space may be narrowed if the clavicle and first rib approximate
- Subaracoid space
- Again, subclavian vessels (artery and vein) and lower roots of brachial plexus can be compressed with tight (shortened) pectoralis minor muscle
What are risk factors for Thoracic Outlet Syndrome?
Congenital abnormalities
- Cervical ribs
- Anomalies of first rib shape, costoclavicular ligament, pectoralis minor or subclavius muscle
- Enlarged scalene tubercle
- Variation in scalene muscle formation and insertion
Trauma
- Whiplash injury with impact to the shoulder or neck
- Bone growth (excessive bone remodelling) after fracture of the clavicle or first rib
- Partial dislocation of the acromioclavicular joint
Soft tissue (Tight, shortened muscles)
- Hypertrophy of the anterior scalene muscle (from heavy weight lifting or faulty breathing pattern e.g. asthma)
- Poor posture, such as forward slouching of the shoulders and forward head carriage
- Occupational stress or sports injury, which involves repetitive overhead movements
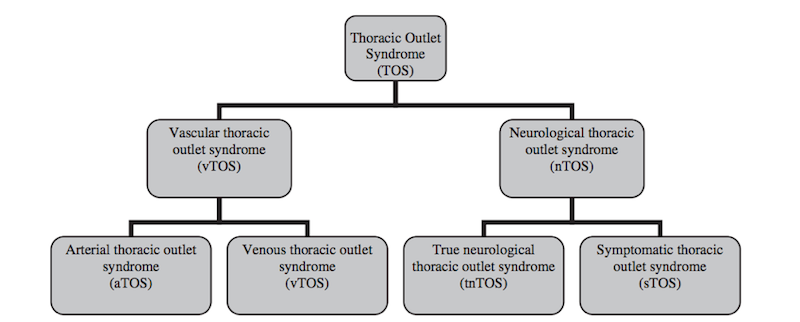
Types of Thoracic Outlet Syndrome
There are two major clinical entities of Thoracic Outlet Syndrome:
- Vascular Thoracic Outlet Syndrome (vTOS)
- Neurological Thoracic Outlet Syndrome (nTOS)
Further classifications are shown in the diagram below
Who is affected by Thoracic Outlet Syndrome?
Approximately 8% of the population is reported to be affected by Thoracic Outlet Syndrome. It predominantly affects young females, and is extremely rare in children. It is reported that 98% of all patients who present in clinic with Thoracic Outlet Syndrome fall into the neurological category.
How do I know if I have Thoracic Outlet Syndrome?
The symptoms which a person experiences with Thoracic Outlet Syndrome depends on which structures in the body are compressed. When nerves are compressed (neurological TOS), the symptoms present as:
- Pain around the neck, shoulder and hand
- Muscle weakness in the base of the thumb and hand (weakened gripping)
- Numbness in the arms and fingers (commonly known as Pins and needles)
Similarly, when vessels are compressed (vascular TOS), symptoms may include:
- Bluish discolouration of the hands (due to inadequate blood supply)
- Pain and swelling in the arm (due to inadequate blood supply and formation of blood clot)
- Cold arms, hands and fingers
- Numbness in the arms and fingers (‘Pins and needles’)
Treatment options for Thoracic Outlet Syndrome
If you are suffering from Thoracic Outlet Syndrome, one thing that you can do to minimise the pain when you are at home is use heat packs, and apply them to the affected area. However, when seeking professional help for Thoracic Outlet Syndrome from practitioners such as a chiropractor or osteopath, techniques that may be used include:
- Muscle stretching and rehabilitation exercise
- Manual therapy including soft tissue release, mobilisation, manipulation and acupuncture
- Behaviour and postural modification
- Medication such as non-steroid anti-inflammatory drugs (NSAIDs), and,
- Surgical intervention, in severe cases
Reference
- Hooper, T. L., Denton, J., McGalliard, M. K., Brismée, J.-M., & Sizer, P. S., Jr. (2010). Thoracic outlet syndrome: a controversial clinical condition. Part 1: anatomy, and clinical examination/diagnosis. Journal of Manual & Manipulative Therapy, 18(2), 74–83.
- Hooper, T. L., Denton, J., McGalliard, M. K., Brismée, J.-M., & Sizer, P. S., Jr. (2010). Thoracic outlet syndrome: a controversial clinical condition. Part 2: non-surgical and surgical management. Journal of Manual & Manipulative Therapy, 18(3), 132–138.
- Ranney, D. (1996). Thoracic outlet: an anatomical redefinition that makes clinical sense. Clinical anatomy (New York, N.Y.), 9(1), 50–52.
- Tariq, M., Zahir, J. and Saleem, S.A., 2000. Role of acupuncture in thoracic outlet syndrome. Acupuncture in Medicine, 18(2), pp.122-123.
- Vanti, C., Natalini, L., Romeo, A., Tosarelli, D. and Pillastrini, P., 2007. Conservative treatment of thoracic outlet syndrome. Eura Medicophys, 43, pp.55-70.
- Watson, L. A., Pizzari, T., & Balster, S. (2009). Thoracic outlet syndrome part 1: clinical manifestations, differentiation and treatment pathways. Man Ther, 14(6), 586–595. doi:10.1016/j.math.2009.08.007
- Watson, L.A., Pizzari, T. & Balster, S., 2010. Thoracic outlet syndrome part 2: conservative management of thoracic outlet. Manual therapy, 15(4), pp.305–14.